This week’s blog is from Randy Jordan, our Chief Advisor for Impact for Health. Randy is a nationally-known community health expert and thought leader who is committed to strengthening and improving healthcare systems, while ensuring that every individual has access to high-quality care.
At the opening of a recent Next Stage staff meeting, the team was asked, “What’s some unfinished business in your career?” After getting over the surprise of such an important question being asked in the icebreaker slot, my answer came immediately to mind – sustainable funding for the safety-net.
My Background
A brief explanation and some background are needed. My professional life began as a pharmacist in a small Florida town where most of my customers were on Medicaid. Even with a Medicaid card, the cost of prescription drugs was a big barrier to my customers receiving their life-saving medications. I did all I could through the use of generic drugs and drug substitution to help them stay drug-compliant, but it was an uphill climb. Why? Because the nature of pharmacy practice was rapidly changing. Local pharmacies were increasingly carrying the banners of large corporations and the prescription drug benefit was more and more controlled by specialized pharmacy benefit managers and mail-order pharmacies. At the same time, drug prices were beginning to skyrocket. My ability as a healthcare professional to influence affordability questions faced by my customers was diminishing day by day.
Healthcare is a Business Opportunity
A version of this story was repeating itself in the lives of other health professionals as the transformation of healthcare from a healing art to a business opportunity began to impact doctors, dentists, nurses, physical therapists and mental health practitioners to name a few. Institutional healthcare providers like hospitals and nursing homes were not immune and faced similar pressures. The last 40 years have been marked by the economic realities of increasing health costs colliding with an elusive desire by healthcare providers to preserve the quality of rendered services.
Sadly, the data from other comparably developed countries suggests that we are losing the cost vs quality battle in the United States. According to a recent Commonwealth Fund report, the United States ranks last among 7 industrialized countries on measures of quality, efficiency, access to care, equity and the ability to lead long, health, and productive lives despite having the most expensive healthcare system.
And, who is really losing out? Underserved, uninsured patients who have been largely left behind in the wake of our country’s healthcare economy.
The growing interests of Medicare, Medicaid and commercial health insurers in transitioning the underlying principles of healthcare to a value-based model have piqued my interest in capitation (fixed per member per month payments) as a provider reimbursement mechanism, especially for healthcare providers dedicated to serving underserved populations. Again, you might ask – Why?
A Capitation Case Study
In the 1990’s, I was a healthcare lawyer specializing in provider risk-sharing arrangements for managed care organizations. I learned from that experience that whoever bore the risk of providing healthcare to a population controlled the way healthcare was delivered. With escalating healthcare costs, health insurance was the dominant player. Capitation was tried and largely failed because of an over-emphasis on cutting healthcare costs at the expense of quality.
In the early 2000s, I shifted to working in the international healthcare space and helped establish 2 charitable hospitals and 3 free clinics in Cambodia, one of the poorest nations in the world. At the time, there was no health insurance in Cambodia and healthcare providers had to make their fixed, global budgets work to continue to serve their patient population. This was a form of capitation surfacing in an unexpected place with a unique twist. The twist was that healthcare in Cambodia was operating with a low-cost structure – allowing providers to adjust their budgets in a way that balanced cost and quality. Amazingly, I experienced hospitals reaching break-even within 5 years and reinvesting their profits into other needed services to benefit their patient population.
So what about today?
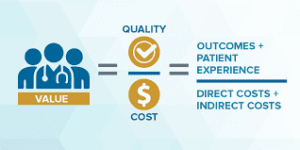
So what about today? I’ve found that North Carolina’s informal safety-net system of healthcare could be an unexpected asset as we strive to achieve the benefits of value-based care. A simple equation helps to illustrate the point: Healthcare Value = Quality divided by Cost.
In the case of safety-net providers, their fixed annual budgets require them to squeeze out excessive costs and maximize the use of their limited resources. As a result, the cost of primary care services among federally qualified health centers is about 75% of the cost of the same services provided through traditional healthcare providers. Among free and charitable clinics, the cost savings are even greater at approximately 50%. Thus, the cost feature of the equation tilts in favor of the safety-net. Quality measures compare favorably too. Comparative quality outcome measures reported by FQHCs and free and charitable clinics are year-on-year on par with or better than the outcomes reported for providers paid through commercial insurance. On the value-based care tally sheet, safety-net providers tick many of the boxes.
Capitating the Safety-Net
When all of this information is taken into account, I’ve found that safety-net primary care providers are ideal candidates for capitation-based reimbursement. It seems counter-intuitive because the safety-net is thinly funded and capitation shifts all the financial risk of providing care from the health insurers to the providers. But, I’m convinced that the safety-net system of healthcare represents a model that provides many advantages: escalating costs are moderated by safety net providers having a history of living within their means and quality performance measures are enhanced because the control of practicing healthcare is placed in the hands of those most highly trained to improve health outcomes.
For me, this remains a bit of unfinished business. If you too are interested in pushing a bit further the idea of seeking sustainable funding for the safety net, feel free to reach out to me at Next Stage – randy@nextstage-consulting.com.